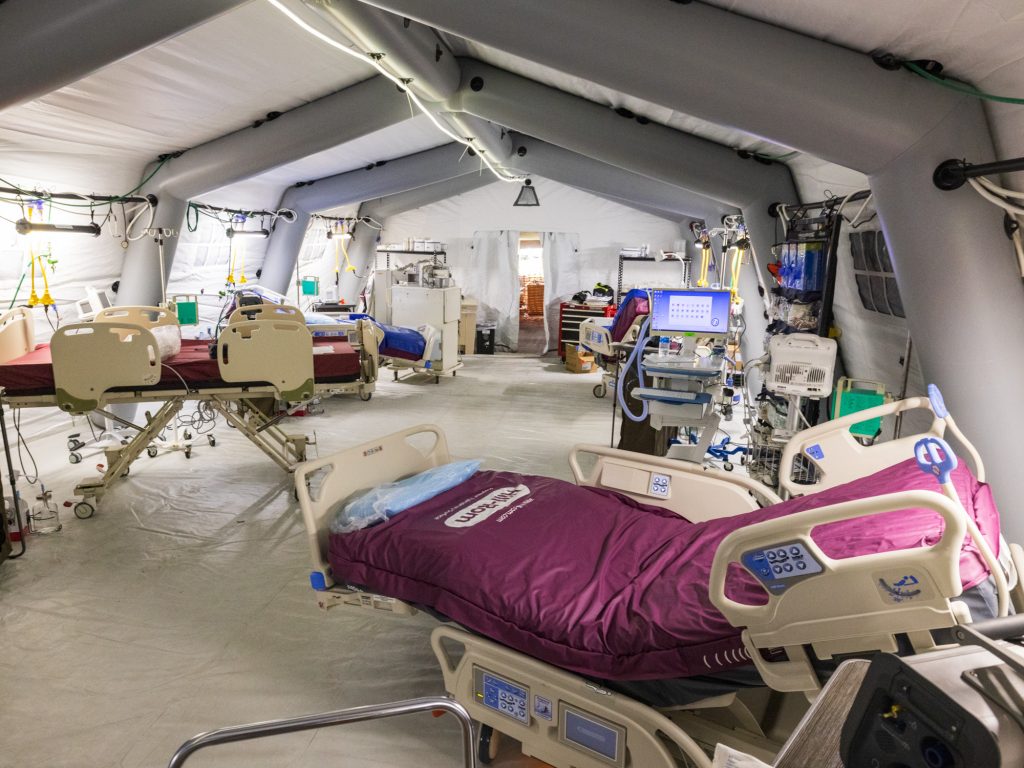
“If we continue that trajectory within the next five to seven to 10 days, I think we’re going to see failure of the hospital system in Mississippi.”
According to Dr. Alan Jones, UMMC Associate Vice Chancellor for Clinical Affairs, the state of Mississippi healthcare is now within the time frame of total collapse since this statement was made just a little over one week ago on August 11, 2021.
That trajectory he mentioned is “the case positivity rate, the rate of new cases, the rate of hospitalizations” occurring during what is now considered the fourth wave of the COVID-19 pandemic. Over the course of a week, Mississippi has broken its own case positivity record five times over with the highest single day number at 5,048, reported on August 19.
The rate of hospitalizations has also increased. There are currently 434 COVID patients in the ICU and 295 patients on ventilators. Dr. Thomas Dobbs, State Health Officer at the MS State Department of Health (MSDH), reports that one-third of ICU patients and two-thirds of those on ventilators will not make it home alive, leaving Mississippi as the #1 hotspot in not just the United States but the world.
WHAT DOES FAILURE OF THE MISSISSIPPI HEALTHCARE SYSTEM MEAN FOR BLACK MISSISSIPPIANS?
From the Trans-Atlantic Slave Trade and into the 21st Century, access to adequate and sustainable healthcare for Black people has fallen short, especially in Mississippi. Before the Civil War, plantation owners covered the bare minimum of healthcare to ensure that enslaved Blacks could continue plowing fields, picking cotton, and tending to any other forms of manual and menial labor. After the Civil War, Blacks were still subject to the harsh conditions of the cotton fields as sharecroppers without as much “protection” from plantation owners.
During Reconstruction, the Freedmen’s Bureau set up hospitals throughout the Confederacy, including Mississippi, treating thousands of Blacks from 1865 to 1869. The state-run hospitals in Vicksburg and Natchez allowed Blacks to receive medical treatment in separate wards from whites. And, for another century, medical care in Mississippi would be segregated.
The revered civil rights activist, Fannie Lou Hamer was unfortunately a prime example of how Blacks, especially Black women, were treated when attempting to receive adequate care. Hamer, who checked herself into a Sunflower County hospital for a minor surgery in 1961, was the ill-fated recipient of a “Mississippi appendectomy” – a practice in which Black women were unknowingly forced into complete hysterectomy procedures. This horrendous racial tactic was used to control the birthrate of Black people.
Although Hamer adopted two girls after the fact, one of her daughters later died of internal hemorrhaging because the Mississippi healthcare system failed to provide adequate healthcare – denied a child adequate healthcare – because of Hamer’s activism. Hamer’s most famous words, “I’m sick and tired of being sick and tired,” were spoken during a time that Medicaid and Medicare were originating in the U.S. healthcare system and gave voice to the centuries of inequities that Blacks experience within that system.
Now, exactly 60 years after Fannie Lou Hamer was coercively given a hysterectomy in a Sunflower County hospital and with the Mississippi healthcare system on the brink of destruction, the inequities in access and information as it pertains to Black people and the healthcare system are still prevalent.
COVID-19 has affected African Americans at an alarmingly disproportionate rate. Though Blacks make up almost 40% of Mississippi’s population, this group accounts for 36% of the COVID cases and 40% of COVID deaths. On a positive note, those trends have gone down from the almost 60% and 70%, respectively, that it was at the beginning of the pandemic.
Nonetheless, underlying issues have made Blacks more susceptible to hospitalizations and deaths due to COVID-19. Economic disparities have made it difficult for some Black people to travel to doctor appointments or to get vaccinated and lack of access to sufficient broadband has made it difficult to take part in the benefits of telehealth and even scheduling vaccination appointments.
Dr. Hursie Sullivan, who is a solo family medicine practitioner in South Jackson, expresses, “Unfortunately, I think there’s always been a schism in the healthcare system in terms of race and delivery of healthcare to communities in Mississippi.” She continues, “I’ve seen the divide or the inequality of that process play out in our communities in terms of health because of access to healthcare. And even sometimes when there’s access, it’s limited. So much goes into [it]. Some people say, well, this group has federal help in terms of health insurance, but they may not have a car to get to the doctor. They may have to pay someone $20, round-trip or each way, to get to the doctor. So, even though they have government assistance in terms of paying, they can’t get to the doctor. A lot of people don’t realize that that is a real factor in administering health.”
Dr. Sullivan also notes that it may be difficult for some families to appropriately quarantine. “If you have 8, 9, or 10 people living in a one-bedroom apartment, when you talk about COVID and you talk about quarantining, or good hand washing, or masking…where are they going to get the money to buy the masks? How do they quarantine in a one-bedroom apartment? Logistically, that’s not realistic. So, potentially, you have an increased risk of exposure to the virus because they can’t go stay at a hotel and quarantine and keep their family safe because that’s the only abode that they have for all seven or eight people. We’re talking generational, multilevel age groups in one setting without the possibility of doing what we suggest. There are other factors that are paramount in receiving healthcare that people don’t consider that I see every day in my practice.”
“WAITING FOR WHAT?”
Despite these disparities, the Black community should still have information readily available to protect themselves. MSDH implores that the number one method to protect one’s self and family from COVID-19 is vaccination. Dr. Sullivan wholeheartedly believes that the vaccine – whether it’s Pfizer, Moderna, or Johnson & Johnson – is one of the number one defenses in preventing the coronavirus from further spreading and mutating, but she has met opposition from patients who are hesitant to get it. “Surprisingly, I’m running into more obstacles in terms of patients who are saying they don’t want to get vaccinated, or they’re thinking about it, or they’re waiting on it. And my question is, ‘waiting for what?’
“The next question that I ask is are there any concerns or questions that you have that I can answer. Initially, people were more likely, in my practice, to want the vaccine. Probably 7 out of 10 people early on in this year were more interested in getting the vaccine. Then, as time has gone on and patients have started to return to the clinic, I have noticed fewer people in my practice alone saying that they were going to get the vaccine and trying to deal with their issues and concerns. A lot of people are getting misinformation from family, friends, and the internet, and they’re sort of passing that stuff on.”
According to MSDH, more than 1,088,000 people have now been fully vaccinated against COVID-19 in Mississippi. There have been massive national, state, and local campaigns to assuage discontent or hesitancy surrounding the vaccine while also providing scientific-based information that dispels the misinformation. In late June, the First Lady of the United States, Dr. Jill Biden, made a special trip to the capital city in a campaign to advise Mississippians to get vaccinated. As a part of that trip, the nation was able to see the work of Jackson’s flagship African American community clinic – Jackson-Hinds Comprehensive Health Center (JHCHC) – in saturating the community with pop-up clinics, including their ongoing partnership with Jackson State University.
Vaccinations are on the upward swing with 71,135 first and second vaccine doses just this week, which is the highest number of vaccine doses since February with 132,042. The lowest number since then was around the Fourth of July holiday with 19,956. And it is suspected that cases related to the Delta variant began to surge around that time as well.
Dr. Jasmine Chapman, CEO of JHCHC, is now seeing about four times as many patients come in to get tested for COVID-19 and an influx of people who are willing to get vaccinated. And she is hopeful in the second medical method of protection against COVID-19 – the monoclonal antibody infusion treatments. These treatments are for COVID positive, symptomatic Mississippians who are not sick enough to be hospitalized. A part of UMMC’s two new field hospitals is set up as a clinic that will offer the monoclonal treatments. And MSDH has ensured that there is no need for a doctor’s visit to receive the treatments.
And, as a community clinic, JHCHC also has been able to administer the monoclonal treatment. Dr. Chapman explains that the treatment is a huge defense in keeping the current structure of the Mississippi healthcare system intact. “That’s what the hospital needs. [They need] the primary healthcare giver – your regular doctor – to begin helping [the hospital system] by treating you early and trying to keep you from even needing to go to a hospital. So the failure is at the hospital level because the primary care level is not overflowed.”
As a primary physician during a point where the healthcare system is breaking down, Dr. Hursie Sullivan notes, “We’re probably going to be more overrun with patients trying to get in who are sicker, who would otherwise, when they’re that sick, go to the emergency room. [They’re] going to feel less compelled to [go to the emergency room] because of the overwhelming surge of the Delta variant. So, people are probably going to move more to the offices and clinics than to the ER. But, ultimately, if people test positive and they’re symptomatic, you want to get them the monoclonal antibody infusion, which then puts it back on the hospital because very few practices, if any, have it available from their facilities.”
As noted previously, JHCHC and UMMC are two of the institutions in the Jackson Metro area that can administer the monoclonal treatments. Dr. Chapman implores, “Whether you’re vaccinated or in the process of getting vaccinated, you should not sit and wait until you get sick. What you need to do immediately once you test positive is you need to call your doctor, and you need to, if you have any type of underlying condition – that could be age, it could be obesity, it could be heart disease – you need to go and get the monoclonal antibody infusion. None of our patients have gone to the hospital or gotten real sick.”
“One of our very first patients was so sick that, to come into the clinic, they had to have help. They could not walk on their own and they got the monoclonal antibody infusion, and when we called them that next morning, that person was up, drinking coffee, and feeling really good. I need everybody to know that they have to ask for it though. The University of Mississippi Medical Center is setting up; the Baptist has it; and JHCHC has a very limited amount.”
To make an appointment with UMMC, visit https://covidmabtreatment.umc.edu. Also, to sign up to receive the COVID-19 vaccine, visit https://www.vaccines.gov/search/. The White House announced at press time that COVID-19 booster shots will be available on September 20 for Americans who received the Pfizer or Moderna vaccines.
The question remains – is the Mississippi health system in failure mode? Dr. Alan Jones stated in a press conference, Tuesday, August 17, “In the systems of care right now, there are, across the state, makeshift ICUs. ICU patients in hallways. ICU patients being held in ERs. Med-surge patients on high flow oxygen and more invasive devices…in terms of the state of the hospital system, we’re standing in a garage with field hospitals. I think that speaks for itself.
“Healthcare in Mississippi is not good right now in terms of what we can do just from the standpoint of being able to care for the patients the way that we as physicians would expect to care for our patients. We’re making the best use of the resources that have been given to us. If people want to know how they can help, go get a vaccine. I hear people say all the time that they want to do their research on the vaccine. Well, I think you should do research about what it would be like to be taken care of in a field hospital in a garage versus getting the vaccine. This is serious business. We are taking care of patients where we’re not normally taking care of patients.”